Frequently Asked Questions – Doctor Clark
Frequently Asked Questions – Doctor Clark
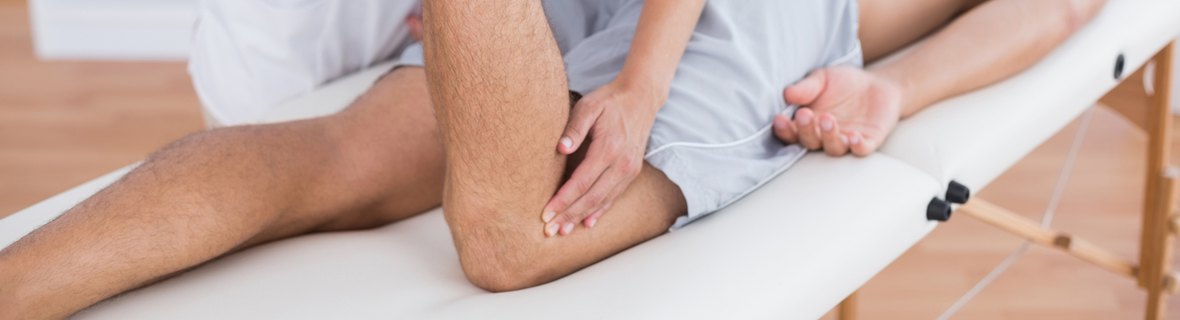
Doctor Clark offers therapies for ligamentous, muscular, myofascial, and joint problems resulting from normal wear-and-tear and and traumatic sprain injuries.

What is the scientific basis for Prolotherapy?
Prolotherapy is an established technique for healing lax, stretched, or torn joint ligaments and muscle tendons. The technique consists of injecting a proliferant solution at the site of attachment of the ligament or tendon to the joint bone.
Read more
Is Prolotherapy an “off-label” use of Procaine™ and Glucose?
Dr. Clark uses the components of the proliferative solution in an “off-label” fashion, extended beyond the usual and customary recommendations of the Federal Drug Administration (FDA).
Read more

To what diagnoses is Prolotherapy applicable?
Prolotherapy is an appropriate therapy for treating any ligament or tendon sprain injury resulting in joint laxity, instability, dysfunction, or pain.
Read more
What is the usual Prolotherapy procedure?
The usual Prolotherapy technique requires delivering a small volume of proliferant solution to the injured ligament or tendon using the following procedure:
Read more
Is Prolotherapy painful?
Injection of the proliferant solution may cause some short-lived pain since the ligaments or tendons are injured and are already tender to needle point.
Read more
What are the frequency and total number of treatment sessions required?
This is always a “crystal ball” prognostication. The extent of treatment required depends on the nature and severity of the patient’s sprain injury and the patient’s musculoskeletal constitution.
Read more
What are the risks of doing no Prolotherapy?
The possible risks of doing no Prolotherapy are:
Read more
What are alternatives to Prolotherapy?
Possible alternatives to Prolotherapy are:
Read more
What are the risks or complications of Prolotherapy?
The potential risks or complications of Prolotherapy are the same as for any medical injection therapy (e.g., flu shot, penicillin shot, cortisone shot):
Read more